Pancreatitis is a medical condition that affects the pancreas, a vital organ responsible for producing digestive enzymes and hormones such as insulin. When the pancreas becomes inflamed, it can lead to a range of health issues.
Understanding Pancreatitis
What is Pancreatitis?
Pancreatitis is the inflammation of the pancreas, a gland located behind the stomach. This inflammation can range from mild to severe and can be acute (sudden and short-term) or chronic (long-lasting).
Causes of Pancreatitis
1. Gallstones
One of the most common causes of acute pancreatitis is the presence of gallstones. When a gallstone blocks the pancreatic duct, it can lead to inflammation.its also common after ERCP.
2. Alcohol Consumption
Excessive alcohol consumption over a long period can irritate and damage the pancreas, leading to chronic pancreatitis.
3. High Triglyceride Levels
Elevated levels of triglycerides, a type of fat in the blood, can increase the risk of pancreatitis.
4. Infections
Certain infections, such as mumps or viral hepatitis, can trigger pancreatitis.
Symptoms of Pancreatitis
1. Abdominal Pain
Severe, persistent abdominal pain(upper abdomin), often radiating to the back, is a hallmark symptom of pancreatitis.Pain is dull, boring, and steady.Pain is sudden in onset and improves with the patient sitting up and bending forward.
2. Nausea and Vomiting
Patients with pancreatitis may experience nausea and vomiting.
3. Fever and Rapid Pulse
Fever and an elevated heart rate are present in 65 percent of patients.
4. Jaundice
Yellowing of the skin and eyes (jaundice) may occur if the inflammation affects the bile duct.
Dyspnea:
May be caused by irritation of the diaphragm (resulting from inflammation), pleural effusion, or a more serious condition, such as acute respiratory distress syndrome (ARDS).It is present in 10 percent of patients.
Hemodynamic Instability
Presented by 10 percent of patients.
Hematemesis or Melena:
Presented by 5 to 10 percent of patients.
Diagnosis
1. Physical Examination For Pancreatitis
Doctors will perform a physical exam to assess the patient’s abdominal tenderness and overall condition.
Cullen sign:
Bluish discoloration around the umbilicus resulting from hemoperitoneum.
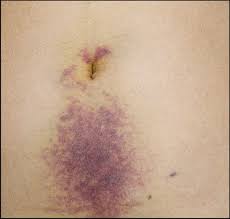
Grey-Turner sign:
it is Reddish-brown discoloration along the flanks.It is due to retroperitoneal blood dissecting along tissue planes.
Erythematous skin nodules:
These may result from focal subcutaneous fat necrosis.Size is usally less then 1cm.These are usually located at extensor surface of skin.
2. Blood Tests
Serum amylase and lipase levels:
Amylase or lipase levels at least 3 times above the reference range are generally considered diagnostic of acute pancreatitis.Mild raised level may indicate only pancreastasis not pancreatitis.Amylase P level are more specific for pancreatitis.
Liver Enzymes
Alkaline phosphatase, total bilirubin, aspartate aminotransferase (AST), and alanine aminotransferase (ALT) levels to search for evidence of gallstone pancreatitis. An ALT level higher than 150 U/L suggests gallstone pancreatitis and a more fulminant disease course.
CBC
it shows leukocytosis (white blood cell [WBC] count higher than 12,000/µL).
Hematocrit value greater than 47% indicates severe disease.
3. Imaging
CT scans and ultrasound can provide detailed images of the pancreas to confirm the diagnosis and assess the severity.
Abdominal ultrasonography For Pancreatitis:
USG abdomen is the most helpful initial test in determining the etiology of pancreatitis and is the technique of choice for detecting gallstones.
CT Scan
CT is generally not indicated for patients with mild pancreatitis unless a pancreatic tumor is suspected.pancreatic tumor is usually present in elderly patients.
Treatment Of Pancreatitis:
Medical management of acute pancreatitis
Medical management of acute pancreatitis is simple.The patient is kept NPO (nil per os—that is, nothing by mouth), and intravenous (IV) fluid hydration is provided. Analgesics are administered for pain relief. Antibiotics are generally not indicated.Patients with acute pancreatitis lose a large amount of fluids to third spacing into the retroperitoneum and intra-abdominal areas. Accordingly, they require intravenous (IV) hydration within the first 24 hours. Especially in the early phase of the illness, aggressive fluid resuscitation is critically important.Resuscitation should be sufficient to maintain hemodynamic stability. This usually involves administration of several liters of fluid as a bolus, followed by continuous infusion at a rate of 250-500 mL/h.
Urine output (>0.5 mL/kg/h) can be followed up as markers of adequate hydration.
- In patients with mild uncomplicated pancreatitis, no benefit is observed from nutritional support, and the energy (caloric) intake received with IV dextrose 5% in water (D5W) suffices; oral feedings should be initiated once the patient’s pain and anorexia resolve
- In patients with moderate-to-severe pancreatitis, begin nutritional support early in the course of management, as soon as stabilization of fluid and hemodynamic parameters permits; optimally, nasojejunal feedings with a low-fat formulation should be initiated at admission
- Total parenteral nutrition (TPN) may be required when patients cannot meet their caloric needs with enteral nutrition or when adequate jejunal access cannot be maintained; the TPN solution should include fat emulsions in amounts sufficient to prevent essential fatty acid deficiency
- If surgery is required for diagnosis or complications of the disease, place a feeding jejunostomy at the time of the operation; use a low-fat formula
- Begin oral feedings once abdominal pain has resolved and the patient regains appetite; the diet should be low in fat and protein
Antibiotics for Acute pancreatitis:
Antibiotics, usually of the imipenem class, should be used in any case of pancreatitis complicated by infected pancreatic necrosis.
1. Hospitalization
Patients with severe acute pancreatitis often require hospitalization to manage symptoms and complications.
2. Fasting
To allow the pancreas to rest and heal, fasting and providing nutrition through intravenous (IV) fluids may be necessary.
3. Pain Management
Pain relief medications are administered to alleviate the severe abdominal pain associated with pancreatitis.
5. Surgery
If ultrasonograms show evidence of gallstones and if the cause of pancreatitis is believed to be biliary, a cholecystectomy should be performed ASAP.
What is Autoimmune pancreatitis?
It is a rare condition. Corticosteroids should not be used to treat this condition in the short term in patients who are suspected of having autoimmune pancreatitis and who present with acute pancreatitis.
